1 of 8
|
Summary of Benefits and Coverage: What this Plan Covers & What You Pay For Covered Services Coverage Period: 09/01/2021 – 08/31/2022
HealthSelect® of Texas (In-Area) Plan Coverage for: Individual + Family Plan Type: POS
The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would
share the cost for covered health care services. NOTE: Information about the cost of this plan (called the premium
1
) will be provided separately.
This is only a summary. For more information about your coverage, or to get a copy of the complete terms of coverage, call 1-800-252-8039 or visit
www.healthselectoftexas.com. For general definitions of common terms, such as allowed amount, balance billing, coinsurance, copayment, deductible, provider, or
other underlined terms see the Glossary. You can view the Glossary at www.healthcare.gov/sbc-glossary/ or call 1-800-252-8039 to request a copy.
Important Questions Answers Why This Matters:
What is the overall
deductible?
Network
$0 Individual / $0 Family
Non-network
$500 Individual / $1,500 Family
Generally, you must pay all of the costs from providers up to the deductible
amount before this plan begins to pay. If you have other family members on the
plan, each family member must meet their own individual deductible until the
total amount of deductible expenses paid by all family members meets the
overall family deductible.
Are there services
covered before you
meet your deductible?
Yes. Preventive services and network services are
covered before you meet your deductible.
In-network and out-of-network COVID-19 diagnostic
testing and related services are covered before you
meet your deductible throughout the Declaration of a
National Emergency due to the novel coronavirus.
This plan covers some items and services even if you haven’t yet met the
deductible amount. But a copayment or coinsurance may apply. For example,
this plan covers certain preventive services without cost sharing and before you
meet your deductible. See a list of covered preventive services at
www.healthcare.gov/coverage/preventive-care-benefits/.
Are there other
deductibles for specific
services?
Yes. $50 for prescription drug expenses per person,
$5,000 for bariatric surgery for active employees, and
$200 per service for certain non-prior authorized
services.
You must pay all of the costs for these services up to the specific deductible
amount before this plan begins to pay for these services.
What is the out-of-
pocket limit for this
plan?
Network
1
: $7,000 Individual / $14,000 Family
Non-network: No Limit
Coinsurance Limit:
$2,000 Network /$7,000 Non-network
The out-of-pocket limit is the most you could pay in a year for covered services.
If you have other family members in this plan, they have to meet their own out-
of-pocket limits until the overall family out-of-pocket limit has been met.
What is not included in
the out-of-pocket limit?
Contributions
2
, balance-billing
3
charges, health care
this plan doesn’t cover, and bariatric surgery benefits.
Even though you pay these expenses, they don’t count toward the out-of-pocket
limit
Will you pay less if you
use a network
provider?
Yes. See www.healthselectoftexas.com or call
1-800-252-8039 for a list of network providers.
This plan uses a provider network. You will pay less if you use a provider in the
plan’s network. You will pay the most if you use an out-of-network provider, and
you might receive a bill from a provider for the difference between the provider’s
charge and what your plan pays (balance billing)
3
. Be aware, your network
provider might use an out-of-network provider for some services (such as lab
work). Check with your provider before you get services.
Do you need a referral
to see a specialist?
Yes. A valid written referral from your primary care
provider is required to see a specialist.
This plan will pay some or all of the costs to see a specialist for covered
services but only if you have an approved referral before you see the specialist.

2 of 8
* For more information about limitations and exceptions, see the plan or policy document at www.healthselectoftexas.com.
\
1 Out-of-pocket limits under this plan reset each calendar year. The network out-of-pocket limit that applies to this plan from 9/1/2021 through 12/31/2021 is $6,750
per Individual and $13,500 per Family
2Under this plan, payment for your health plan coverage is called a contribution rather than a premium.
3
Non-network providers may not balance bill you for certain services effective January 1, 2020. Refer to the Master Benefit Plan Document for details.
All copayment and coinsurance costs shown in this chart are after your deductible has been met, if a deductible applies.
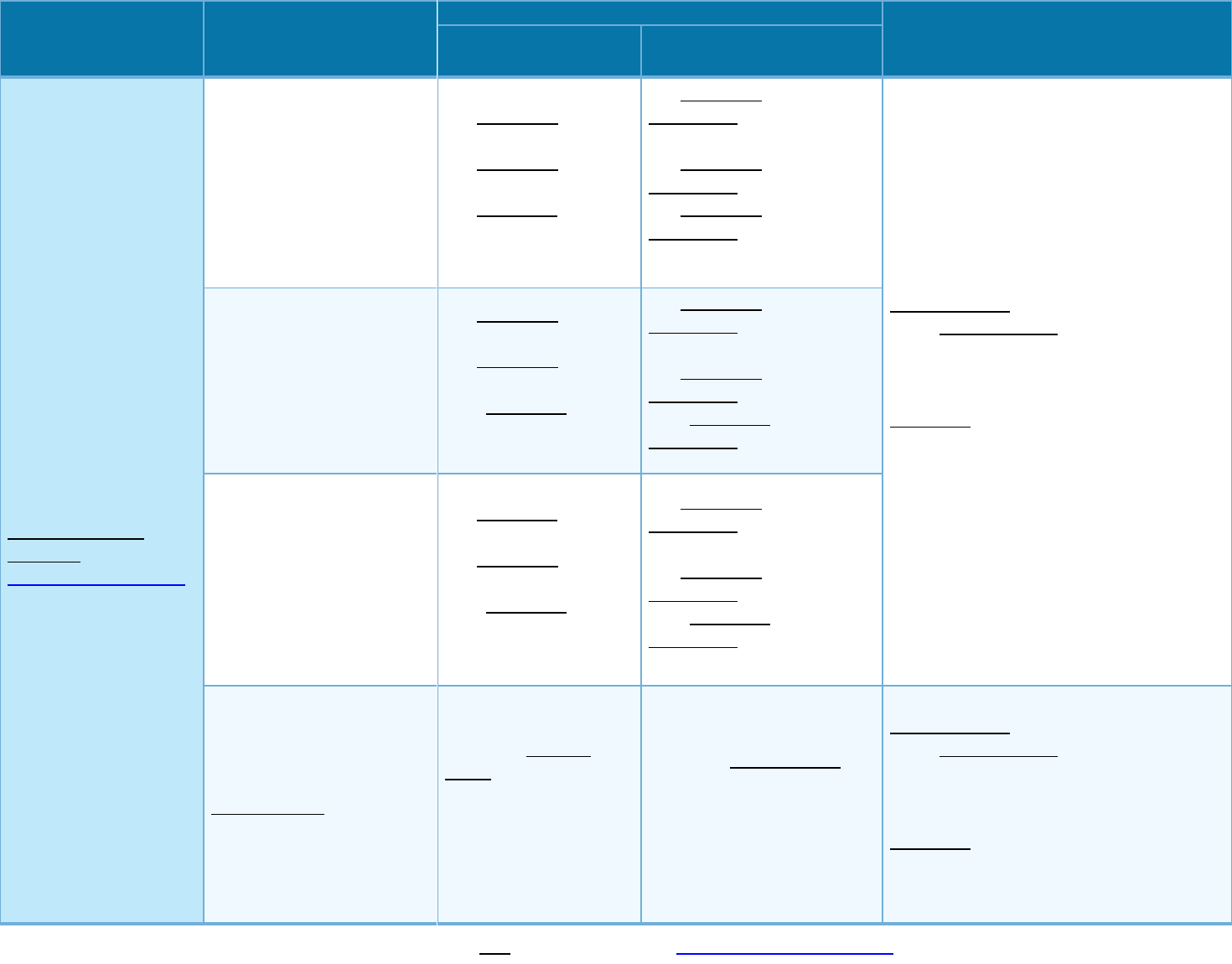
Common
Medical Event
Services You May Need
What You Will Pay
Limitations, Exceptions, & Other
Important Information
In-Network Provider
(you will pay the least)
Out-of-Network Provider
(you will pay the most)
If you visit a health care
provider’s office or
clinic
Primary care visit to treat an
injury or illness
$25 copayment/visit 40% coinsurance
In-network and out-of-network COVID-19
diagnostic testing and related services are
covered without cost share throughout the
Declaration of a National Emergency due to
the novel coronavirus.
Specialist visit $40 copayment/visit 40% coinsurance
A valid referral to see a network specialist
(including telemedicine visits) is required to
access network benefits excluding
OB/Gynecologists, chiropractors, and eye
exams by ophthalmologists and optometrists.
In-network and out-of-network COVID-19
diagnostic testing and related services are
covered without cost share throughout the
Declaration of a National Emergency due to
the novel coronavirus.
Preventive care/screening/
Immunization
No charge 40% coinsurance
You may have to pay for services that aren’t
preventive. Ask your provider if the services
needed are preventive. Then check what
your plan will pay for.
If you have a test
Diagnostic test (x-ray, blood
work)
20% coinsurance 40% coinsurance
In-network and out-of-network COVID-19
diagnostic testing and related services are
covered without cost share throughout the
Declaration of a National Emergency due to
the novel coronavirus.
Imaging (CT/PET scans,
MRIs)
$100 copayment/visit
plus 20% coinsurance
$100 copayment/visit
plus 40% coinsurance
Preauthorization may be required. Failure to
obtain preauthorization may increase your
cost.

3 of 8
* For more information about limitations and exceptions, see the plan or policy document at www.healthselectoftexas.com.
Common
Medical Event
Services You May Need
What You Will Pay
Limitations, Exceptions, & Other
Important Information
In-Network Provider
(you will pay the least)
Out-of-Network Provider
(you will pay the most)
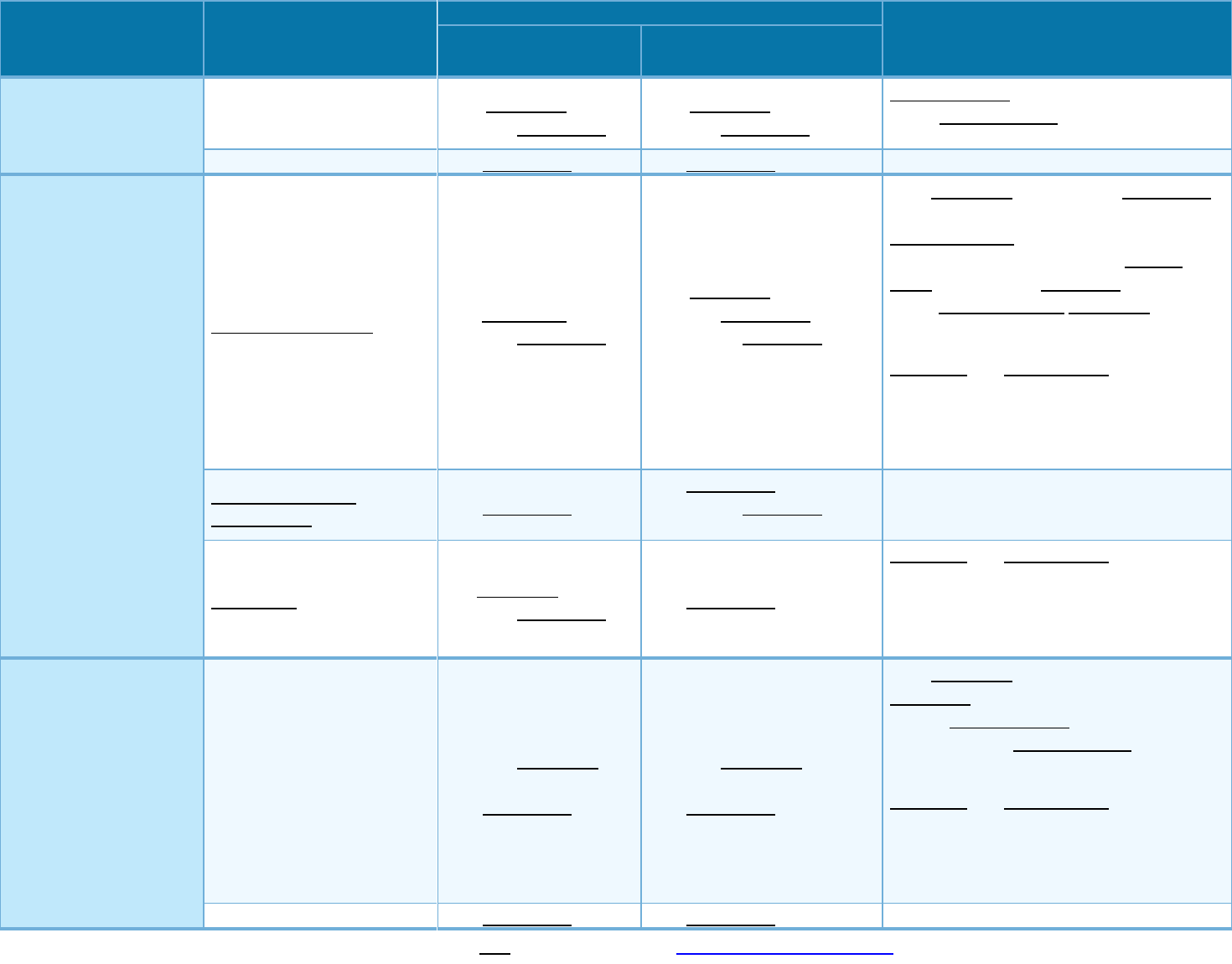
If you need drugs to
treat your illness or
condition
More information about
prescription drug
coverage is available at
www.healthselectrx.com.
Generic drugs (Tier 1)
$10 copayment (non-
maintenance),
$10 copayment
(maintenance);
$30 copayment
(mail order or extended
day supply)
$10 copayment plus 40%
coinsurance
(non-maintenance)
$10 copayment plus 40%
coinsurance (maintenance);
$30 copayment plus 40%
coinsurance
(mail order or extended day
supply)
Preauthorization may be required. Failure to
obtain preauthorization may increase your
cost. Note: If a generic drug is available and
you choose to buy the preferred or non-
preferred brand drug, you will pay the generic
copayment plus the cost difference between
the preferred or non-preferred brand drug
and the generic drug.
Preferred brand drugs (Tier 2)
$35 copayment (non-
maintenance),
$45 copayment
(maintenance);
$105 copayment (mail
order or extended day
supply)
$35 copayment plus 40%
coinsurance
(non-maintenance)
$45 copayment plus 40%
coinsurance (maintenance);
$105 copayment plus 40%
coinsurance (mail order or
extended day supply)
Non-preferred brand drugs
(Tier 3)
$60 copayment
(non-maintenance),
$75 copayment
(maintenance);
$180 copayment (mail
order or extended day
supply)
$60 copayment plus 40%
coinsurance
(non-maintenance)
$75 copayment plus 40%
coinsurance (maintenance);
$180 copayment plus 40%
coinsurance (mail order or
extended day supply)
Specialty drugs
If purchased through a
pharmacy, specialty
drugs are covered as
preferred brand drugs or
non-preferred brand
drugs as listed above.
Otherwise, covered as a
medical benefit.
If purchased through a
pharmacy, specialty drugs are
covered as preferred brand
drugs or non-preferred brand
drugs as listed above.
Otherwise, covered as a
medical benefit.
Preauthorization may be required. Failure to
obtain preauthorization may increase your
cost. Note: If a generic drug is available and
you choose to buy the preferred or non-
preferred brand drug, you will pay the generic
copayment plus the cost difference between
the preferred or non-preferred brand drug
and the generic drug.

4 of 8
* For more information about limitations and exceptions, see the plan or policy document at www.healthselectoftexas.com.
Common
Medical Event
Services You May Need
What You Will Pay
Limitations, Exceptions, & Other
Important Information
In-Network Provider
(you will pay the least)
Out-of-Network Provider
(you will pay the most)
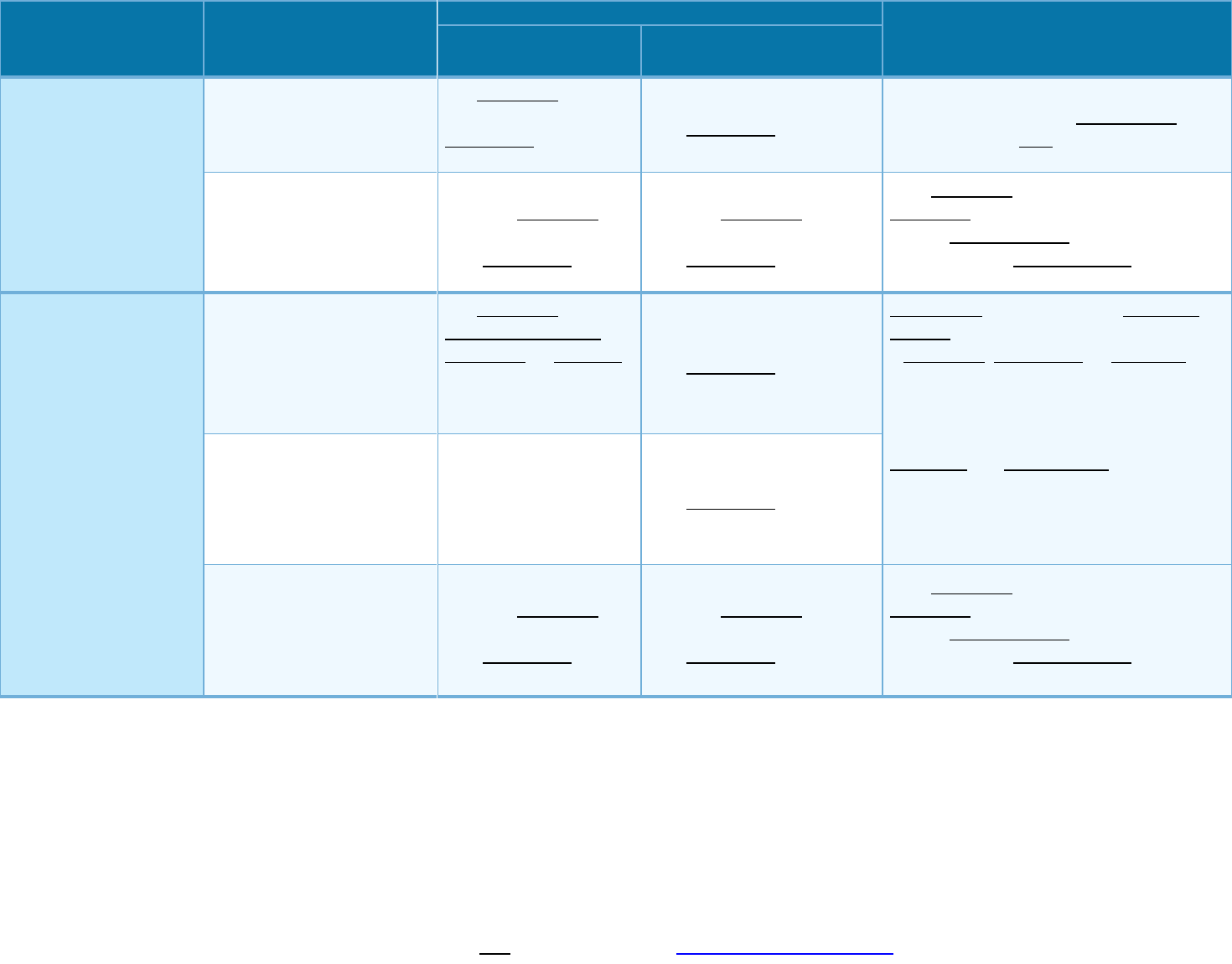
If you have outpatient
surgery
Facility fee (e.g., ambulatory
surgery center)
$100 copayment/visit
plus 20% coinsurance
$100 copayment/visit
plus 40% coinsurance
Preauthorization may be required. Failure to
obtain preauthorization may increase your
cost.
Physician/surgeon fees 20% coinsurance 40% coinsurance None
If you need immediate
medical attention
Emergency room care
$150 copayment/visit
plus 20% coinsurance
$150 copayment/visit
plus 20% coinsurance
Non-network deductible does
not apply
$300 copayment/visit plus 20% coinsurance
applies to any non-network freestanding
emergency room not affiliated with a hospital,
and you may be responsible for balance
billing
3
. Non-network deductible does not
apply. Emergency room copayment waived if
admitted.
In-network and out-of-network COVID-19
diagnostic testing and related services are
covered without cost share throughout the
Declaration of a National Emergency due to
the novel coronavirus.
Emergency medical
transportation
20% coinsurance
20% coinsurance
Non-network deductible does
not apply
None
Urgent care
$50 copayment/ visit
plus 20% coinsurance
40% coinsurance
In-network and out-of-network COVID-19
diagnostic testing and related services are
covered without cost share throughout the
Declaration of a National Emergency due to
the novel coronavirus.
If you have a hospital
stay
Facility fee (e.g., hospital
room)
$150/day copayment per
admission plus
20% coinsurance
$150/day copayment per
admission plus
40% coinsurance
$750 copayment max per admission. $2,250
copayment max per calendar year per
person. Preauthorization may be required.
Failure to obtain preauthorization may
increase your cost.
In-network and out-of-network COVID-19
diagnostic testing and related services are
covered without cost share throughout the
Declaration of a National Emergency due to
the novel coronavirus.
Physician/surgeon fees 20% coinsurance 40% coinsurance None

5 of 8
* For more information about limitations and exceptions, see the plan or policy document at www.healthselectoftexas.com.
Common
Medical Event
Services You May Need
What You Will Pay
Limitations, Exceptions, & Other
Important Information
In-Network Provider
(you will pay the least)
Out-of-Network Provider
(you will pay the most)
If you need mental
health, behavioral
health, or substance
abuse services
Outpatient services
$25 copayment for office
visits and 20%
coinsurance for other
outpatient services
40% coinsurance
Certain services must be preauthorized; refer
to Master Benefit Plan Document for details.
Inpatient services
$150/day copayment per
admission plus
20% coinsurance
$150/day copayment per
admission plus
40% coinsurance
$750 copayment max per admission. $2,250
copayment max per calendar year per
person. Preauthorization may be required.
Failure to obtain preauthorization may
increase your cost.
If you are pregnant
Office visits
$25 copayment for
primary care provider/$40
copayment for specialist
for initial office visit
No Charge after initial
visit
40% coinsurance
Cost sharing does not apply for preventive
services. Depending on the type of services,
a copayment, coinsurance, or deductible may
apply. Maternity care may include tests and
services described elsewhere in the SBC (i.e.
ultrasound.)
In-network and out-of-network COVID-19
diagnostic testing and related services are
covered without cost share throughout the
Declaration of a National Emergency due to
the novel coronavirus.
Childbirth/delivery
professional services
No Charge 40% coinsurance
Childbirth/delivery facility
services
$150/day copayment per
admission plus
20% coinsurance
$150/day copayment per
admission plus
40% coinsurance
$750 copayment max per admission. $2,250
copayment max per calendar year per
person. Preauthorization may be required.
Failure to obtain preauthorization may
increase your cost.

6 of 8
Common
Medical Event
Services You May Need
What You Will Pay
Limitations, Exceptions, & Other
Important Information
In-Network Provider
(you will pay the least)
Out-of-Network Provider
(you will pay the most)
If you need help
recovering or have
other special health
needs
Home health care 20% coinsurance 40% coinsurance
Preauthorization may be required. Failure to
obtain preauthorization may increase your
cost. Max of 100 non-network visits per
calendar year per person. Non-network home
infusion therapy is not covered.
Rehabilitation services 20% coinsurance 40% coinsurance
None
Habilitation services 20% coinsurance 40% coinsurance
Skilled nursing care 20% coinsurance 40% coinsurance
Preauthorization may be required. Failure to
obtain preauthorization may increase your
cost.
Durable medical equipment 20% coinsurance 40% coinsurance
Repair or replacement limit of one every 3
years per person unless change in condition
or physical status. Preauthorization may be
required. Failure to obtain preauthorization
may increase your cost.
Hospice services 20% coinsurance 40% coinsurance
Preauthorization may be required. Failure to
obtain preauthorization may increase your
cost.
If your child needs
dental or eye care
Children’s eye exam $40 copayment/visit; 40% coinsurance
Limit of one routine exam per calendar year
per person. No referral is required for eye
exams. One preventive care visual acuity
screening covered with no copayment at
network provider.
Children’s glasses Not covered Not covered None
Children’s dental check-up Not covered Not covered None
Excluded Services & Other Covered Services:
Services Your Plan Generally Does NOT Cover (Check your policy or plan document for more information and a list of any other excluded services.)
• Acupuncture
• Cosmetic surgery
• Dental care (Adult)
• Educational services, excluding Diabetes Self-
Management Training Programs
• Glasses and Contact Lenses
• Infertility treatment
• Long-term care
• Personal comfort items
• Routine foot care
* For more information about limitations and exceptions, see the plan or policy document at www.healthselectoftexas.com.

7 of 8
Other Covered Services (Limitations may apply to these services. This isn’t a complete list. Please see your plan document.)
• Bariatric surgery for active employees
• Chiropractic care
• Hearing aids (limited to $1,000 per ear
per 36-month period) Eligible minors
18 and under are not subject to $1,000
hearing aid maximum
• Non-emergency care when traveling outside the U.S.
• Private-duty nursing (limited to 96 hours per year for non-
network)
• In-network diagnostic mammograms are covered at 100%
• Routine eye care (Adult)
• Weight loss programs (Limited to certain
programs. See Master Benefit Plan Document for
details on covered programs)
Your Rights to Continue Coverage: There are agencies that can help if you want to continue your coverage after it ends. The contact information for those
agencies is: the HealthSelect of Texas plan at 1-800-892-2803, U.S. Department of Labor’s Employee Benefits Security Administration at 1-866-444-EBSA (3272) or
www.dol.gov/ebsa/healthreform, or Department of Health and Human Services, Center for Consumer Information and Insurance Oversight, at 1-877-267-2323
x61565 or www.cciio.cms.gov. Other coverage options may be available to you too, including buying individual insurance coverage through the Health Insurance
Marketplace. For more information about the Marketplace, visit www.HealthCare.gov or call 1-800-318-2596.
Your Grievance and Appeals Rights: There are agencies that can help if you have a complaint against your plan for a denial of a claim. This complaint is called a
grievance or appeal. For more information about your rights, look at the explanation of benefits you will receive for that medical claim. Your plan documents also
provide complete information to submit a claim, appeal, or a grievance for any reason to your plan. For more information about your rights, this notice, or assistance,
contact: Blue Cross and Blue Shield of Texas at 1-800-252-8039 or visit www.healthselectoftexas.com, or contact the U.S. Department of Labor's Employee Benefits
Security Administration at 1-866-444-EBSA (3272) or visit www.dol.gov/ebsa/healthreform. Additionally, a consumer assistance program can help you file your
appeal. Contact the Texas Department of Insurance's Consumer Health Assistance Program at 1-800-252-3439 or visit www.texashealthoptions.com.
Does this plan provide Minimum Essential Coverage? Yes
If you don’t have Minimum Essential Coverage for a month, you’ll have to make a payment when you file your tax return unless you qualify for an exemption from the
requirement that you have health coverage for that month.
Does this plan meet the Minimum Value Standards? Yes
If your plan doesn’t meet the Minimum Value Standards, you may be eligible for a premium tax credit to help you pay for a plan through the Marketplace.
Language Access Services:
Spanish (Español): Para obtener asistencia en Español, llame al 1-800-252-8039.
Tagalog (Tagalog): Kung kailangan ninyo ang tulong sa Tagalog tumawag sa 1-800-252-8039.
Chinese (中文): 如果需要中文的帮助,请拨打这个号码 1-800-252-8039.
Navajo (Dine): Dinek'ehgo shika at'ohwol ninisingo, kwiijigo holne' 1-800-252-8039.
To see examples of how this plan might cover costs for a sample medical situation, see the next section.

8 of 8
About these Coverage Examples:
This is not a cost estimator. Treatments shown are just examples of how this plan might cover medical care. Your actual costs will be
different depending on the actual care you receive, the prices your providers charge, and many other factors. Focus on the cost sharing
amounts (deductibles, copayments and coinsurance) and excluded services under the plan. Use this information to compare the portion of
costs you might pay under different health plans. Please note these coverage examples are based on self-only coverage.
Peg is Having a Baby
(9 months of in-network pre-natal care and a
hospital delivery)
◼ The plan’s overall deductible $0
◼ Specialist copayments $40
◼ Hospital (facility) coinsurance 20%
◼ Hospital (facility) copayments $150
◼ Other coinsurance 20%
This EXAMPLE event includes services like:
Specialist office visits (prenatal care)
Childbirth/Delivery Professional Services
Childbirth/Delivery Facility Services
Diagnostic tests (ultrasounds and blood work)
Specialist visit (anesthesia)
Total Example Cost $12,700
In this example, Peg would pay:
Cost sharing
Deductibles $10
Copayments $400
Coinsurance $2,200
What isn’t covered
Limits or exclusions $60
The total Peg would pay is $2,670
Managing Joe’s type 2 Diabetes
(a year of routine in-network care of a well-
controlled condition)
◼ The plan’s overall deductible $0
◼ Specialist copayments $40
◼ Hospital (facility) coinsurance 20%
◼ Other coinsurance 20%
This EXAMPLE event includes services like:
Primary care physician office visits (including
disease education)
Diagnostic tests (blood work)
Prescription drugs
Durable medical equipment (glucose meter)
Total Example Cost
$5,600
In this example, Joe would pay:
Cost sharing
Deductibles $50
Copayments $900
Coinsurance $0
What isn’t covered
Limits or exclusions $20
The total Joe would pay is $970
Mia’s Simple Fracture
(in-network emergency room visit and follow
up care)
◼ The plan’s overall deductible $0
◼ Specialist copayments $40
◼ Hospital (facility) coinsurance 20%
◼ Hospital (ER) copayments $150
◼ Other coinsurance 20%
This EXAMPLE event includes services like:
Emergency room care (including medical
supplies)
Diagnostic test (x-ray)
Durable medical equipment (crutches)
Rehabilitation services (physical therapy)
Total Example Cost $2,800
In this example, Mia would pay:
Cost sharing
Deductibles $10
Copayments $400
Coinsurance $400
What isn’t covered
Limits or exclusions $0
The total Mia would pay is $810
The plan would be responsible for the other costs of these EXAMPLE covered services.

If
you,
or
someone
you
are
helping,
have
questions,
you
have
the
right
to
get
help
and
information
in
your
language
at
no
cost
To
speak
to
an
interpreter,
call
the
customer
service
number
on
the
back
of
your
member
card.
If
you
are
not
a
member,
or
don't
have
a
card,
call
855-710-6984.
Si
usted
o
alguien
a
quien
usted
está
ayudando
tiene
preguntas,
tiene
derecho
a
obtener
ayuda
e
información
en
su
idioma
sin
costo
alguno.
Para
hablar
con
un
intérprete
comuniqúese
con
el
número
del
Servicio
al
Cliente
que
figura
en
el
reverso
de
su
tarjeta
de
miembro.
Si
usted
no
es
miembro
o
no
posee
una
tarjeta,
llame
al
855-710-6984.
bcbstx.com

.
Health care coverage is important for everyone.
We provide free communication aids and services for anyone with a disability or who needs language assistance.
We do not discriminate on the basis of race, color, national origin, sex, age or disability.
To receive language or communication assistance free of charge, please call us at 855-710-6984.
If you believe we have failed to provide a service, or think we have discriminated in another way, contact us to file a grievance.
Office of Civil Rights Coordinator
300 E. Randolph St.
35th Floor
Chicago, IL 60601
Phone: 855-664-7270 (voicemail)
TTY/TDD: 855-661-6965
Fax: 855-661-6960
You may file a civil rights complaint with the U.S. Department of Health and Human Services, Office for Civil Rights, at:
U.S. Dept. of Health & Human Services
200 Independence Avenue SW
Room 509F, HHH Building 1019
Washington, DC 20201
Phone: 800-368-1019
TTY/TDD: 800-537-7697
Complaint Portal: https://ocrportal.hhs.gov/ocr/portal/lobby.jsf
Complaint Forms: http://www.hhs.gov/ocr/office/file/index.html
